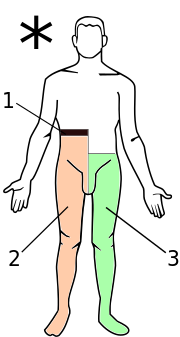
Brown-Séquard syndrome
| |||||||||
Read other articles:

Peta Senonges. Senonges merupakan sebuah komune di departemen Vosges yang terletak pada sebelah timur laut Prancis. Lihat pula Komune di departemen Vosges Referensi INSEE lbsKomune di departemen Vosges Les Ableuvenettes Ahéville Aingeville Ainvelle Allarmont Ambacourt Ameuvelle Anglemont Anould Aouze Arches Archettes Aroffe Arrentès-de-Corcieux Attignéville Attigny Aulnois Aumontzey Autigny-la-Tour Autreville Autrey Auzainvilliers Avillers Avrainville Avranville Aydoilles Badménil-aux-Boi...

Caspar HedioBiografiKelahiran1494 (Kalender Masehi Gregorius) Ettlingen Kematian17 Oktober 1552 (Kalender Masehi Gregorius) (57/58 tahun)Strasbourg Cathedral preacher (en) Data pribadiAgamaGereja Lutheran PendidikanUniversitas Albert Ludwig Freiburg KegiatanPekerjaanSejarawan dan teolog Caspar Hedio, ukiran tembaga abad ke-16 Caspar Hedio, juga ditulis sebagai Kaspar Hedio, Kaspar Heyd, Kaspar Bock atau Kaspar Böckel (Ettlingen, 1494 - Strasbourg, 17 Oktober 1552) adalah se...

Model berpose di studio foto. Fotogenik (dari bahasa Yunani φωτογενής fotogenís) adalah istilah untuk penampilan wajah dan sikap tubuh yang menghasilkan potret yang menyenangkan.[1] Wajah yang fotogenik tidak serta-merta berarti secara estetis proporsional. Wajah fotogenik tidak lebih merupakan wajah yang tampak bagus ketika difoto.[2] Daya tarik fisik Keadaan fotogenik dapat berhubungan atau tidak berhubungan dengan daya tarik fisik seseorang di dunia nyata. Model u...

The neutrality of this article is disputed. Relevant discussion may be found on the talk page. Please do not remove this message until conditions to do so are met. (June 2016) (Learn how and when to remove this template message) Economy of KazakhstanDowntown AstanaCurrencyTenge (KZT, ₸)Fiscal yearcalendar yearTrade organizationsWTO, CIS, EAEU, EACU, ECO, SCO, CISFTACountry group Developing/Emerging[1] Upper-middle income economy[2] StatisticsPopulation 20,050,032 (2024 est....

Halaman ini berisi artikel tentang perintah Allah. Untuk ritual dalam Yudaime, lihat Bar Mitvah dan Bat Mitzvah. Orang Yahudi Agama Yahudi Agama Tuhan Allah dalam Yudaisme Dasar Iman Yahudi Kaballah Hari raya Doa Halakha Mitzvot (Daftar: 613) Rabi Sinagoge Pembacaan gulungan Taurat Minhag/Kebiasaan Tzedakah Teks Tanakh: Taurat Nevi'im Ketuvim Literatur Rabinik Talmud Mishnah Gemara Etnis Ashkenazi Sefardim Mizrahi Beta Israel Penduduk (Daftar) Israel AS Rusia/Uni Soviet SpanyolKanada Jerman P...

في الاقتصاد، الفائدة المركبة (بالإنجليزية: Compound interest) تنشأ عندما تجمع الفائدة إلى المبلغ الأصلي، ومن تلك اللحظة يحق للفائدة بالإضافة إلى المبلغ الأصلي principal تجميع فائدة خلال فترة لاحقة.[1][2][3] وتسمى إضافة الفائدة إلى المبلغ الأصلي تركيب الفائدة مع المبلغ الأص...

Federasi Sepak Bola KosovoUEFADidirikan1946Kantor pusatPristinaBergabung dengan FIFA2016Bergabung dengan UEFA2016Websiteffk-kosova.com Federasi Sepak Bola Kosovo (bahasa Albania: Federata e Futbollit e Kosovës; bahasa Serbia: Фудбалски савез Косова / Fudbalski savez Kosova) adalah badan pengendali sepak bola di Kosovo,[1] dengan kantor pusat di Pristina. Federasi Sepak Bola Kosovo didirikan pada tahun 1946 sebagai cabang dari Asosiasi Sepak Bola Yugoslavia...

Cet article est une ébauche concernant un historien. Vous pouvez partager vos connaissances en l’améliorant (comment ?) selon les recommandations des projets correspondants. Karl BrandiBiographieNaissance 20 mai 1868MeppenDécès 9 mars 1946 (à 77 ans)GöttingenSépulture StadtfriedhofNationalité allemandeFormation Gymnasium Carolinum (en)Activités Médiéviste, historien moderniste, professeur d'universitéFratrie Ernst Brandi (en)Autres informationsA travaillé pour Univer...

لاسانا فاني معلومات شخصية الاسم الكامل لاسانا فاني الميلاد 11 نوفمبر 1987 (العمر 36 سنة)باماكو، مالي الطول 6 قدم 0 بوصة (1.83 م) مركز اللعب وسط الجنسية مالي مسيرة الشباب سنوات فريق 2001–2005 دجوليبا المسيرة الاحترافية1 سنوات فريق م. (هـ.) 2006–2009 دجوليبا 63 2009–2010 المريخ الرياض...

Open air entertainment venue For other uses, see Amphitheatre (disambiguation). The Colosseum, an amphitheatre in Rome (built 72–80 AD) An amphitheatre (British English) or amphitheater (American English; both /ˈæmfɪˌθiːətər/)[1][2] is an open-air venue used for entertainment, performances, and sports. The term derives from the ancient Greek ἀμφιθέατρον (amphitheatron),[3] from ἀμφί (amphi), meaning on both sides or around[4] and θέ...

Alessandro Borghese - Celebrity ChefPaeseItalia Anno2022 - in produzione Generereality, talent show, cucina Edizioni3 Puntate144 (al 25 aprile 2024) Durata60 min Lingua originaleitaliano RealizzazioneConduttoreAlessandro Borghese RegiaGianni Monfredini AutoriAlessandro Borghese (st. 1-2) Monia Palazzo (st. 1-2)Nicola Lorusso (st. 1)Laura Cristaldi (st. 1)Antonio Moreno (st. 1)Marco Soprano (st. 2)Sonia Soldera (st. 2) Casa di produzioneSky Brand Solutions con Banijay Studios Italy Ret...

Pour les articles homonymes, voir Liège (homonymie). Liège au Portugal. Le liège est un produit agricole et un matériau cellulaire, produit à partir de l'écorce du chêne-liège. Cet arbre est actuellement le seul produisant des quantités exploitables de suber, même si ce tissu végétal est présent dans toutes les plantes vasculaires et parfois en quantité remarquée comme chez le phellodendron. Le suber protège l'arbre des insectes, du froid, des intempéries, et des incendies, ...

Questa voce o sezione sull'argomento centri abitati dell'Umbria non cita le fonti necessarie o quelle presenti sono insufficienti. Commento: Non sono citate le fonti storiografiche. Puoi migliorare questa voce aggiungendo citazioni da fonti attendibili secondo le linee guida sull'uso delle fonti. Castiglione del Lagocomune Castiglione del Lago – Veduta LocalizzazioneStato Italia Regione Umbria Provincia Perugia AmministrazioneSindacoMatteo Burico (PD) dal 27-5...

Road in Los Angeles, California Obama BoulevardNamesakeBarack ObamaMaintained byLos Angeles Department of TransportationLength3.5 miles (5.6 km)LocationLos Angeles, CaliforniaWest endCulver City city limit near Ballona CreekEast endExposition Boulevard in Leimert Park, Los Angeles President Barack Obama Boulevard (commonly known as Obama Boulevard) is a major thoroughfare in South Los Angeles. It stretches 3.5 miles (5.6 km) from Baldwin Hills (past Baldwin Village and Cre...

The Alhama River The Alhama is a tributary of the Ebro. Its source is Suellacabras, in Soria, and it flows for 78 kilometres (48 mi) until it reaches the Ebro at Alfaro (La Rioja). See also List of rivers of Spain 42°11′02″N 1°43′05″W / 42.1839°N 1.7181°W / 42.1839; -1.7181 This article related to a river in Spain is a stub. You can help Wikipedia by expanding it.vte

У этого термина существуют и другие значения, см. Бэтмен (значения). У этого термина существуют и другие значения, см. Брюс Уэйн (значения). Бэтменангл. Batman Изображение с обложки выпуска Batman № 608 (октябрь 2002, второе издание) Художник — Джим Ли Контурщик — Скотт Уильямс �...

Foro de las Naciones Libres Posrusas Tipo organización políticaFundación 8 de mayo de 2022Personas clave Räfis QaşapofVadim ShtepaPavlo KlimkinJaroslav RomanchukTaras StećkiwAnna FotygaOleg MagaletskyJanusz BugajskiPaul A. GobleAjmed ZakáyevKosma ZłotowskiAnders ÅslundEdward LucasGiulio Terzi Di Sant'AgataGianni VernettiIlya PonomarevTaras KuzioFrédéric PetitSyreś Boläeńsin etiquetarRuslan GabbasovSitio web freenationsrf.org[editar datos en Wikidata] El Foro de las Nac...

يفتقر محتوى هذه المقالة إلى الاستشهاد بمصادر. فضلاً، ساهم في تطوير هذه المقالة من خلال إضافة مصادر موثوق بها. أي معلومات غير موثقة يمكن التشكيك بها وإزالتها. (نوفمبر 2019) دوري قيرغيزستان لكرة القدم 1998 تفاصيل الموسم دوري قيرغيزستان لكرة القدم النسخة 7 البلد قيرغيزستان&#...

Guillaume Du Fay Nama dalam bahasa asli(fr) Guillaume Dufay BiografiKelahiran13 Agustus 1397 Beersel (Kadipaten Brabant) Kematian27 November 1474 (Kalender Masehi Gregorius) (77 tahun)Cambrai (Kekaisaran Romawi Suci) KegiatanSpesialisasiMusik dan teori musik Pekerjaankomponis, music theorist (en) Periode aktif1420 (Kalender Masehi Gregorius) –GenrePolifoni dan musik klasik AliranBurgundian School (en) Karya kreatifKarya terkenal Missa Se la face ay pale (en) Missa L'Homme armé (e...

Japanese commander In this Japanese name, the surname is Taira. Sammichūjō Koremori woodblock print by Utagawa Yoshitora, 1866. Taira no Koremori (平 維盛) (1158 – 1184) was one of the Taira clan's commanders during the Genpei War of the late Heian period of Japanese history. He was the only child of Taira no Shigemori, who was the eldest regent and heir of Taira no Kiyomori.[1] Early life Taira no Koremori was born in 1158.[1] In contrast to his father, who was a warri...